Contributors: Deanna Banks, Jessica Homann, and Kevin Reddy
Our executive talent experts share the latest trends in healthcare leadership to help you navigate the future, despite political uncertainty. Discover leadership skills and strategies that propel organizations forward as care delivery shifts beyond traditional settings.

The healthcare industry is undergoing a profound transformation amid never-before-seen challenges and pressures aimed at all aspects of its ecosystem. Ever-evolving political agendas and policy shifts continue to create significant uncertainty around Medicare and Medicaid programs, both of which have been under stress for some time. Artificial intelligence is revolutionizing care delivery, refining services, and, in some cases, moving beyond traditional settings, while persistent staffing shortages and financial pressures strain health systems to their limits.
As margins tighten and federal funding undergoes new constraints and evolving requirements, organizations confront fundamental questions about their future. Leaders must simultaneously navigate political landscapes, drive innovation, strengthen workforce culture, and maintain fiscal stability – all while delivering exceptional patient care in an increasingly complex regulatory environment.
With so many variables at play, we are experiencing some of the highest levels of turmoil and ambiguity since the COVID-19 pandemic. New concerns are being added to the top of the stack daily.
The healthcare industry serves an increasingly multifaceted population across geographical, socioeconomic, racial, ethnic, gender, and ability dimensions. This reality presents both an opportunity and an imperative for organizations to build high-performing leadership teams and a workforce that reflects and understands the communities they serve.
High-functioning organizations recognize that multidimensional leadership teams drive better health outcomes, enhance patient experience, and strengthen financial performance through more effective, accessible care delivery.
Pair all of that with ongoing challenges around workforce, care delivery, and major shifts in market paradigms, and you’ve got a recipe for an extremely volatile outlook:
- Recent policy changes and ongoing federal budget pressures are reshaping Medicare and Medicaid programs, with implications such as:
- Stricter Medicare Advantage plan oversight affecting payer operations and compliance costs
- Medicaid funding reductions leading to state-level eligibility restrictions and benefit reductions
- Pressure on DSH (Disproportionate Share Hospital) payments threatens safety-net hospital sustainability
- Accelerated push toward value-based payment models to contain costs
- Disproportionate impact on rural and critical access health systems already operating with a minimal financial cushion
- Strategic provider-payer partnerships emerging as organizations seek to navigate funding constraints
- Federal spending reductions, including significant Medicaid cuts and changes to National Institutes of Health (NIH) funding, threaten organizational stability and research capabilities
- Clinical workforce challenges intensify as physicians face Medicare reimbursement shortfalls, mounting administrative burden, and staffing shortages – all while managing evolving patient expectations
- Care delivery continues to evolve beyond traditional hospital settings toward homes, retail locations, and outpatient facilities, driven by AI, clinical innovations, and changing consumer preferences
- Heightened regulatory oversight emerges across multiple fronts – from state-level scrutiny of non-profit tax exemptions to increased restrictions on private equity ownership
- Market disruption accelerates through industry consolidation, retail health providers entering the space, and recent private equity-backed healthcare organization bankruptcies reshaping competitive dynamics
Strategic Priorities for Healthcare Leadership
Financial concerns remain a pressing theme in leadership discussions across all sectors of the healthcare ecosystem. Changes to federal spending and policies have the potential to destabilize many organizations. Academic medical centers, in particular, feel these pressures as they navigate changes to NIH funding that could impact their research programs, talent recruitment, and role in driving medical innovation. Leaders must develop strategies to maintain organizational stability while preserving their institutions’ core missions amid this uncertainty.
Complexity around Medicare funding, scrutiny of Medicare Advantage plans, and evolving price transparency requirements further complicate the situation. Meanwhile, staffing shortages persist and are exacerbated by ongoing challenges, including burnout and turnover, administrative complexity, and evolving patient expectations, prompting them to rethink their approaches to retention and team culture.
Key Executive Leadership Qualities that Drive Success
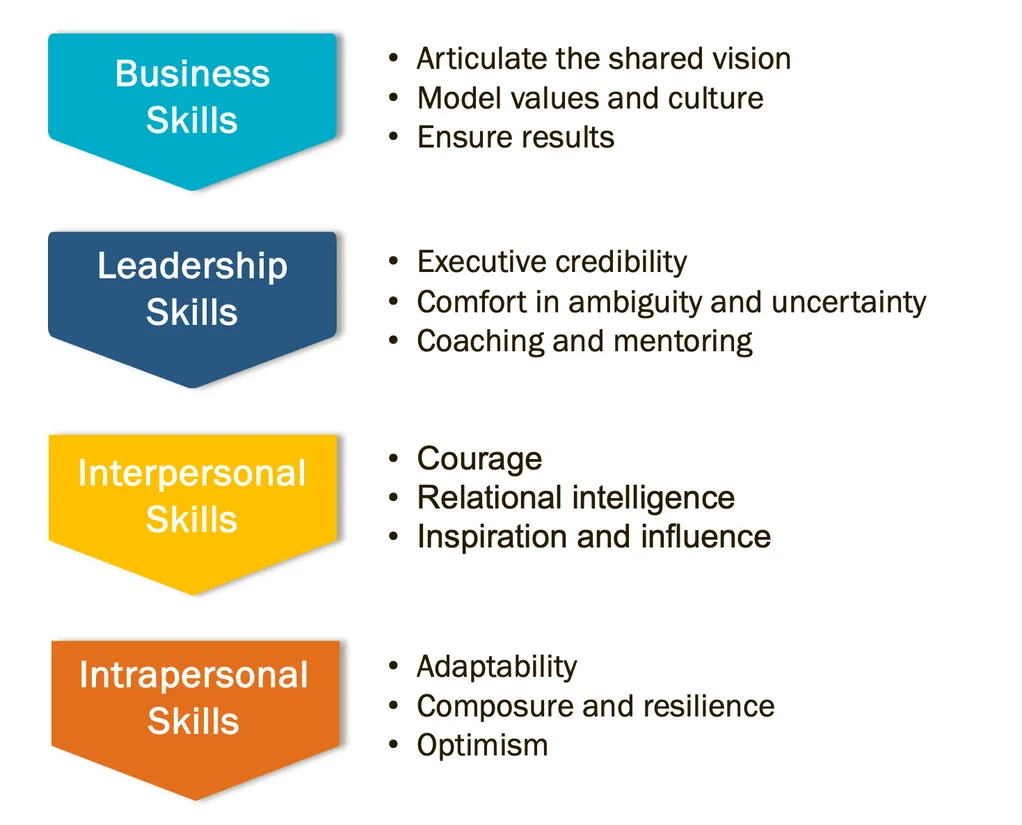
This tumultuous environment calls for leaders who can master multiple domains. “Healthcare executives require a blend of skills across business acumen, leadership, and interpersonal and intrapersonal abilities,” says Jessica Homann, Vice President of Furst Group. This combination provides the necessary skills to navigate an intricate web of new technologies, processes, partnerships, and regulations while managing finite resources, including the energy and well-being of themselves and their team members.
Deanna Banks, Principal of Furst Group and NuBrick Partners, points to fundamental changes in workforce expectations and organizational culture. “Leaders are encountering mounting pressures to develop talent and shape culture in an environment where many roles have gone remote or hybrid,” states Deanna. “This comes at a time when organizations are already strained by increased demand and decreased workforce availability.”
To achieve sustainable success, healthcare executives must possess a well-balanced blend of business and leadership skills, while continually honing and enhancing their emotional intelligence.
Strategic Leadership Competencies
1. Industry Knowledge and Strategic Vision
Successful leaders must possess deep industry knowledge and strategic foresight. As Deanna notes: “Only those who are acutely knowledgeable of the healthcare industry and possess the acumen to anticipate trends, shifts in the regulatory environment, opportunities to develop partnerships and/or sunset unprofitable ones while balancing market disruption largely spawned by private equity will remain.”
2. Regulatory Navigation and Governance
The regulatory landscape grows increasingly complex as states examine tax exemptions for non-profit hospitals and legislators seek greater oversight of private equity ownership in healthcare. Executives must also navigate evolving requirements around mental health parity enforcement, site-neutral payments, and price transparency, all of which impact operational strategies and revenue models.
Leaders in this environment must demonstrate expertise in:
- Maintaining organizational compliance while driving innovation
- Building sustainable governance models
- Managing diverse stakeholder relationships
- Balancing community benefit with financial sustainability
- Adapting business models to new payment and pricing requirements
- Ensuring equitable access across service lines including mental health
3. Innovation and Adaptability
C-Suite leaders must be adept at driving meaningful change while maintaining operational excellence. Kevin Reddy, Principal of Furst Group, emphasizes that organizations want “leadership talent who understand the dynamics of the healthcare system and who have the capacity to think outside the traditional format to bring new ideas to effect efficiencies and lower costs without sacrificing quality and access to care.”
4. Trust and Psychological Safety
Creating an environment of trust and open communication is crucial for organizational success. In reference to the chart above, Jessica Homann underscores the power of leadership courage with two emerging executive competencies: “Displaying openness and humility” and “Putting principles first.” She stresses how top leaders create environments where “people feel safe to share candid feedback and ideas, as well as to take risks and try new things.”
The Transformation of Healthcare Delivery
Healthcare delivery continues to experience disruption, with clinical innovations and AI pushing some aspects of care away from traditional hospital settings into homes, pharmacies, outpatient facilities, and physicians’ offices. This fundamentally changes what, where, how, and who delivers care. Retail health providers and technology companies are emerging as significant market players, creating new competitive dynamics and partnership opportunities.
These changes demand leaders who can:
- Reimagine care delivery models while maintaining quality and access
- Build strategic partnerships across traditional and new healthcare settings
- Navigate complex relationships with emerging market participants
- Balance innovation with organizational stability
What’s Next – 3 Key Shifts
Leaders stand at a critical juncture as they prepare for the transformative changes ahead. Shifts in payment models, workforce dynamics, and technological integration will fundamentally reshape healthcare delivery. Organizations anticipating and adapting to these changes will be better positioned to thrive in an increasingly complex environment.
As health systems look ahead, three key developments emerge as central to leadership strategy:
1. Value-Based Healthcare Evolution
The healthcare industry continues to move toward value-based care models that prioritize outcomes. Kevin Reddy, Principal of Furst Group, envisions a future characterized by “The principles of the quintuple aim, where a focus on improving patient experience, population health, reducing costs, improving clinician experience, and increasing health equity will drive enhanced collaboration among stakeholders, with providers and payers joining forces to establish equitable reimbursement based on quality outcomes and stakeholder value.” This evolution occurs against a backdrop of Medicare drug price negotiations and site-neutral payment discussions, requiring leaders who comprehend both the clinical and business impacts of new payment models.
Deanna emphasizes that “This comprehensive transformation demands leaders who can reconcile innovation with stability, digital acceleration with human connection, and financial sustainability with quality care.”
2. Strategic Workforce Development
Organizations are placing increased emphasis on building and maintaining strong teams. Kevin notes that “developing and training the workforce for the future is a strategic imperative” as competition for talent intensifies.
Focusing on this aspect is vital, particularly as clinical staff experience a plethora of challenges and impacts to work expectations. Furthermore, leaders are pressured to sustain team engagement and foster positive dynamics. External factors like government regulations and executive orders that affect operations and ongoing internal organizational needs to deliver on business objectives through the continued integration of multidimensional talents and perspectives are challenging organizational priorities.
This dynamic environment presents complex challenges across all leadership levels. Physicians, now predominantly employed by hospitals, face mounting frustration with Medicare reimbursement structures and expanding administrative responsibilities. Meanwhile, clinical teams continue to navigate persistent labor shortages while managing increasing patient expectations and administrative workload.
At the executive level, leaders must balance these clinical workforce dynamics with broader organizational demands, including digital transformation, financial sustainability, and strategic partnerships. This multifaceted environment requires leaders who can foster supportive organizational cultures, drive innovation, and maintain operational efficiency while ensuring high-quality care delivery. Success increasingly depends on executives who can bridge the gap between clinical and business priorities, building teams that are both highly engaged and high-performing.
3. Digital Transformation
“Several transformative trends are reshaping healthcare leadership requirements,” shares Deanna Banks, Principal – Furst Group and NuBrick Partners. “Artificial intelligence is at the forefront, revolutionizing everything from clinical decision-making to operational efficiency. This digital transformation extends beyond AI to encompass telemedicine, digital health records, and health equity initiatives, requiring leaders who can drive technological integration while focusing on quality care delivery.”
Technology integration and digital transformation remain core components of a robust business strategy. Deanna emphasizes the importance of leaders embracing technology through telemedicine, digital health records, health and wellness education, and promoting health equity. Additionally, the push toward home-based care and retail health settings further accelerates this digital evolution.
Building Future-Ready Teams
Sustainable success now demands executives who excel at balancing competing priorities while sparking innovation and maintaining stability. Beyond traditional management skills, leaders must master the integration of technology, change leadership, emotional intelligence, and strategic foresight. Those who thrive will stay nimble and forward-looking while keeping quality care and the health and well-being of their teams at the center of their focus.
Building effective, high-performing executive leadership teams takes an intentional approach. Furst Group’s commitment to human-centered leadership means supporting organizational transformation through:
- Creating pathways for meaningful connection and growth
- Building teams that reflect and understand their communities
- Supporting authentic, empathetic leaders and organizations
- Measuring impact through both human and business outcomes
Strong multidimensional leaders and teams drive more substantial business outcomes, higher employee engagement, and enhanced talent retention. Connect with us to access tools and strategies for accelerating your team’s performance.
Additional Resources for Action:
Professional Assessment Algorithm – How to Win The Talent War
Servant Leadership: Valuing Relationships over Process
Case Study: 5 Signs Your Leadership Team Needs Acceleration
Survey Report: Healthcare Leadership Lessons from the COVID-19 Pandemic
15 Values-Based Interview Questions that Identify Authentic Leadership
Trends Shaping the Future of Palliative Care, PACE, and Post-Acute
Webinar: Supercharge Team Performance with a Feedback-Centric Culture